This is where design comes in—and why a nurse’s insight is invaluable on our healthcare design teams. As with triage, we have been programming and adapting our clients’ ED spaces for some time—beyond just designating a room in accordance with state-of-the-practice guidelines (see the Joint Commission on Accreditation of Healthcare Organizations and the Facilities Guidelines Institute). Having an RN at the table facilitates these collaborations between our designers and our clients, so that their healthcare environments can always deliver, no matter how fast a virus mutates, a policy changes, or a new resource becomes available.
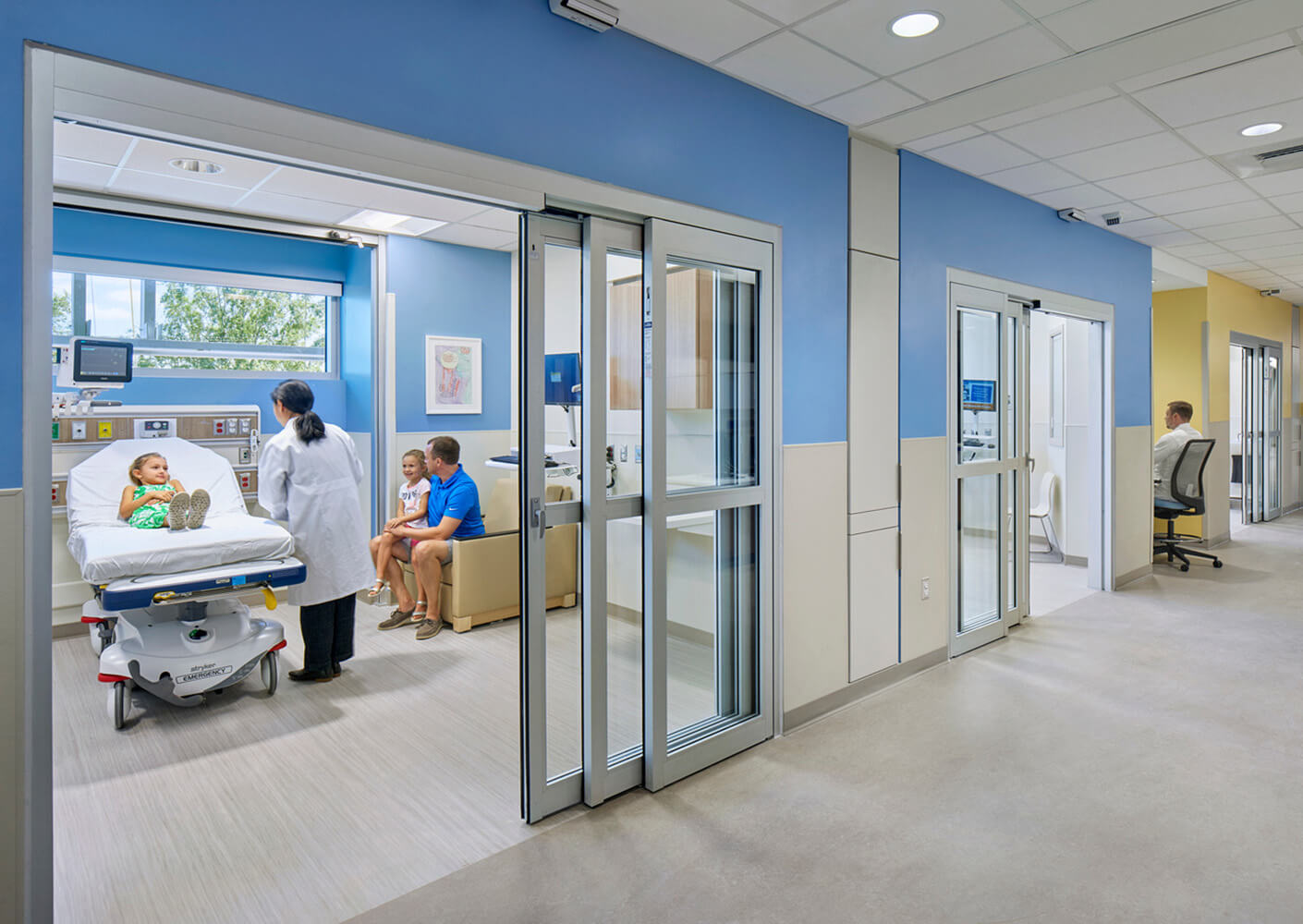
Until EDs cease to be the only option for people not adequately covered by health insurance, we will continue to help our clients respond strategically and empathically to initiatives like the new crisis hotline. De-escalation Rooms, Flex Rooms, and Behavioral Health Modules, shown below, are a few of the ED solutions we have been innovating with consideration for the client’s budget, capacity, demand, and population.
Look out next week for more insights on the crisis hotline and healthcare design from our colleague Sabah Mohammed, who just completed her E. Todd Wheeler Health Fellowship report, “Care in the Time of Crisis: Designing for Patients with Behavioral Health Needs in the Emergency Department.”