1. Reducing Stigma: Behavioral healthcare centers will take a stronger, more proactive role in transforming the way society views mental health treatment. Integration with the community, public education and awareness, post-treatment patient support networks, and the implementation of “telemedicine” systems (whereby health services are delivered via electronics and telecommunications platforms) will reduce the stigma associated with mental health patients and their treatment.
2. Calming Emergency Departments: The same warm, open, light-filled designs we see in behavioral health centers will be incorporated into emergency departments to create a more inclusive, accepting environment that allows patients to feel safe. Open team stations will replace those surrounded by windows. Distraction walls—designed to calm patients by taking their minds off the fact that they are in a clinical setting—will be incorporated.
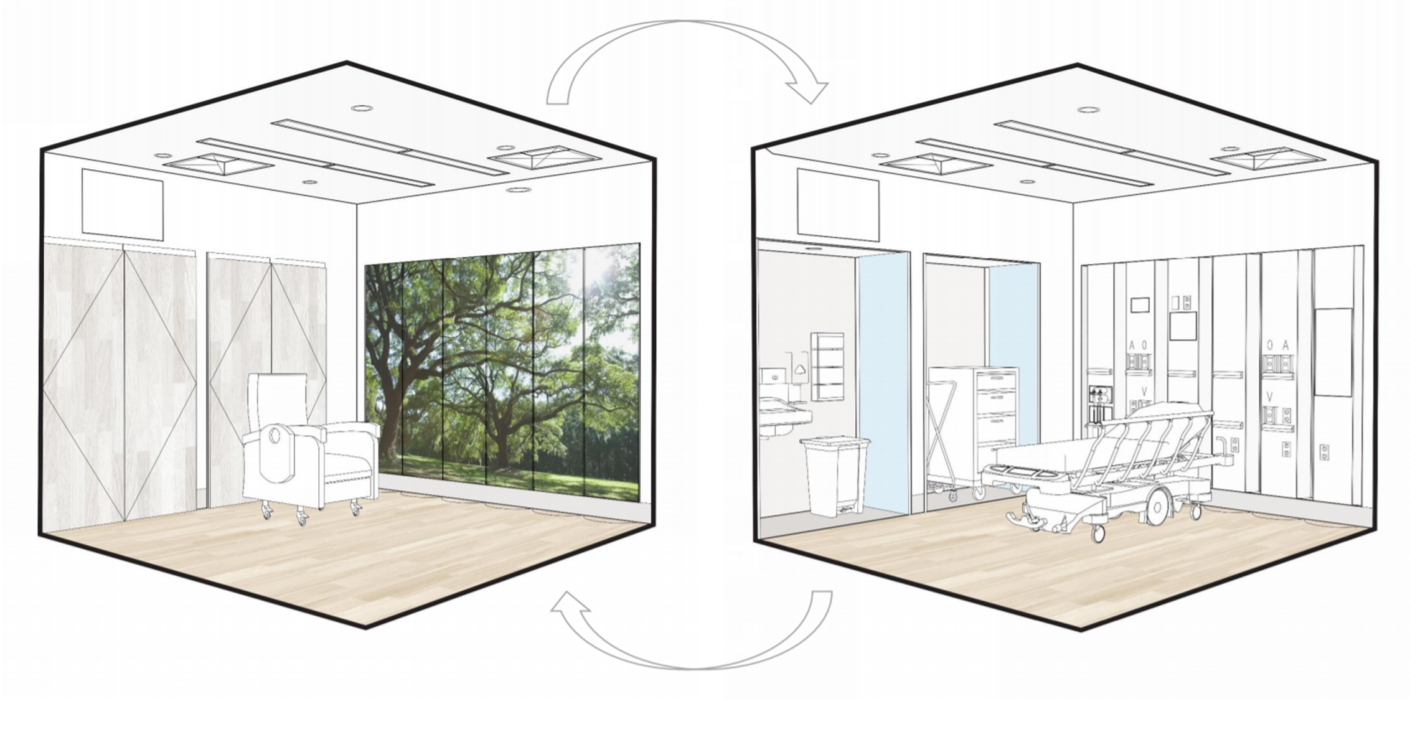
3. Adaptable Treatment Rooms: Emergency department treatment rooms will be designed to flex to respond to cases on a sliding scale of emergency severity. Headwalls with rotating panels that lock into place will allow for multiple variations of treatment that are customizable to the patient’s needs. For example, one side of the panel might display a custom-printed image of a natural landscape, thereby serving as a distraction wall; the other side of the panel would house clinical tools, including medical gasses, pumps, power, and monitoring. By designing treatment rooms that adapt to serve patients with medical health needs, behavioral health needs, or both, an increased number of patients will be accommodated more efficiently.