This project posed several unique challenges:
The Sherman Center Street Campus had been closed for half a decade. After the demolition of the inpatient hospital years prior, the campus operated as an outpatient facility that included operating and imaging rooms and as a medical office building. Very few rooms were suitable for ACF patient use. Walking into a building that has been unoccupied for years is always a window into a previous point in the building’s life: you can see the passage of time. For this building, that meant finding abandoned supplies, equipment and furniture in most rooms and significant water damage and mold. Knowing there were four weeks for cleanup and conversion felt like the challenge of a lifetime.
The quick turnaround – 26 days – and availability of materials were central challenges. The trade partners identified available materials and equipment, and the architect/engineer team reviewed options with the trade partners to find the right solution using what could be delivered and installed within the timeframe available. This high level of coordination ensured a smooth process.
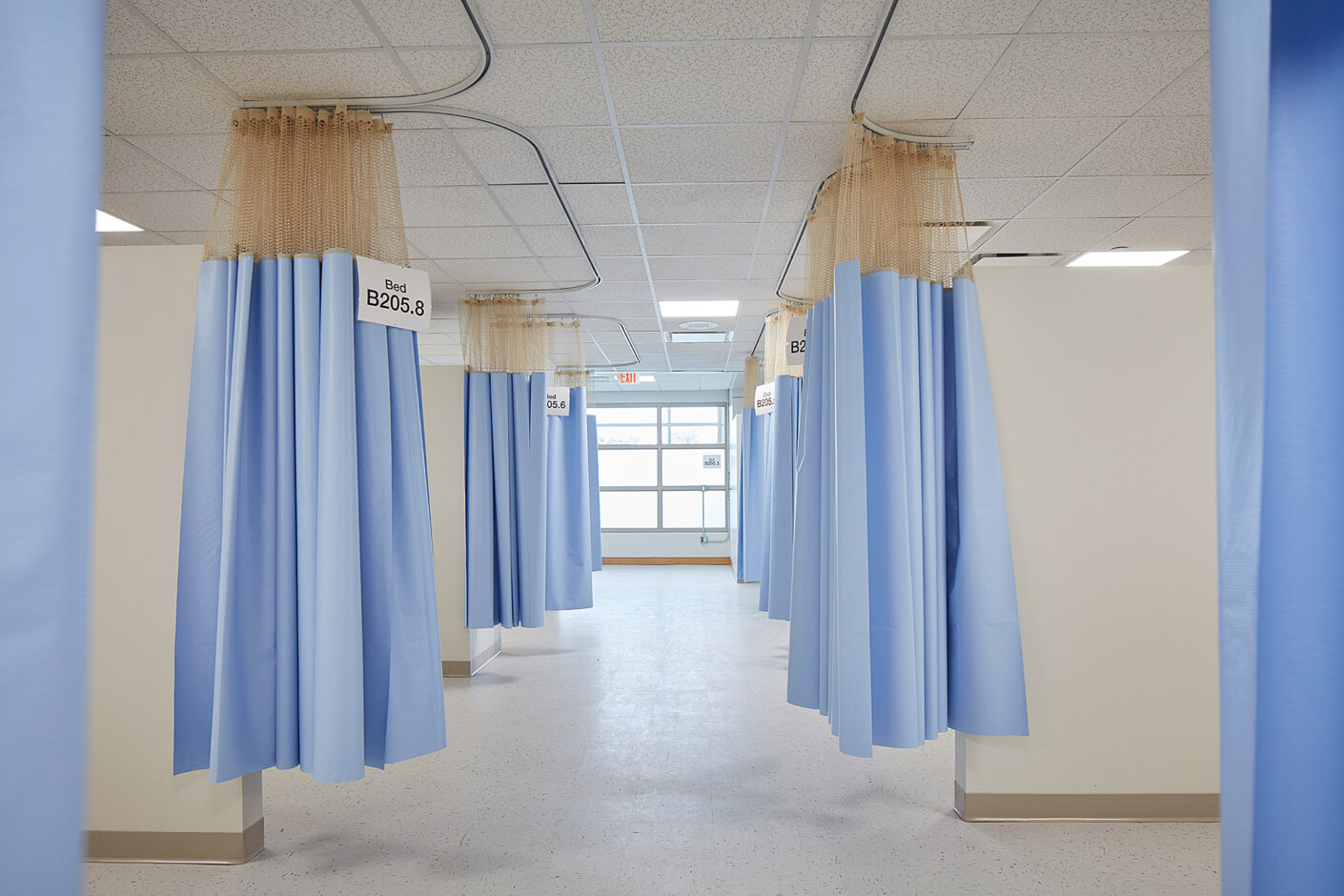
In the first days on site, we determined that some demolition would be required to optimize the bed count. Our initial goal was to limit demolition and use existing spaces as much as possible: limiting reconstruction would be most time efficient. However, with the help of superintendents from Turner and the subcontractors, we quickly realized that wholesale interior demolition would be the most efficient solution in the southern zone of the building. This approach allowed for more beds by creating an “open ward” concept with 3-sided walled patient positions. Opening the floor plan also increased nursing visibility into patient bays, which would not have been possible with the existing cellular nature of the prior medical office space. This same area was converted to a negative pressure zone to increase patient comfort. With natural light at the perimeter now penetrating the entire unit, this zone of the building received a facelift that would not have been possible without extensive demolition.
Early in the project, we used a bay module with CDC–recommended bed clearances to evaluate whether an existing space could adequately house a bed. By mapping out all available existing locations, we determined a target bed count. During the first week, the Design-Build team and the USACE team continuously evaluated space conditions and tested infrastructure approaches to refine the bed count. Clinical guidance from regular visits by IDPH further informed decisions. As Turner Construction and our trade partners generated cost information, planning decisions were re-evaluated and the plan was adjusted.